|
Thus the evidence level provides an orientation of the effectiveness of the therapeutic option which, however, must be critically questioned by the treating physician. This classification is made based on a gradient: the higher the classification of evidence, the better the scientific justification for a resulting treatment recommendation. The classification of evidence into evidence levels is an important aspect of evidence-based medicine. The basis is the most recent status of clinical medicine and published clinical trials that confirm or disprove an option. Hereby, the currently best evidence for or against decisions in the treatment of the individual patients should be applied. Today, evidence-based medicine means that decisions of medical treatment are made patient-oriented, possibly based on empirically proven effectiveness. Those publications led to an increasing acceptance of clinical epidemiology. Feinstein with his publication entitled “Clinical Judgement” that appeared in 1967 and on the publication of the British epidemiologist Archie Cochrane entitled “Effectiveness and efficiency: random reflections on health services”. Furthermore, it is based on the work of the American physician and mathematician Alvan R. The current evidence-based medicine is based among others on the work of David Sackett who was lecturer at the Department of Clinical Epidemiology and Biostatistics of the McMaster University, Hamilton, Canada, as founding director. According to recent knowledge, the term of “evidence in medicine” was first used in 1793 by the Scottish physician George Fordyce. Instead, an empirically elaborated evidence should be applied which is generated by means of scientific studies and systematic observation. The idea of evidence-based medicine can already be found in the 18 th century when British physicians developed the concept of “medical arithmetic” requiring abandonment of superstition and renunciation of useless drugs in the conception of therapeutic approaches. 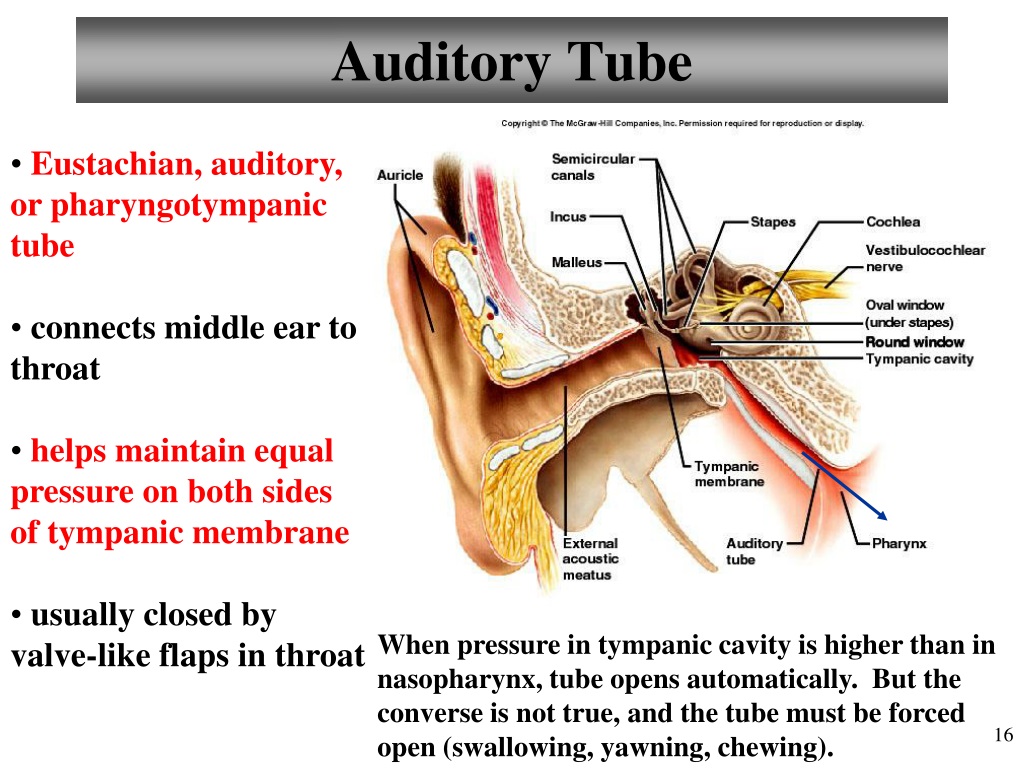
Otitis media, Eustachian tube dysfunction, evidence, evidence gaps, antibiotic therapy If this need is addressed, a wealth of implications can be expected for therapeutic approaches in the years to come. Numerous evidence-based studies are therefore necessary in order to evaluate the evidence pertaining to existing and future therapy solutions for impaired middle ear ventilation and otitis media. Owing to the multitude of variables, the classification of evidence levels for various treatment approaches calls for highly diversified assessment. There is, as yet, no evidence for some of the other long-established procedures. More recent procedures such as balloon dilation of the Eustachian tube have also shown initial success but must undergo further evaluation with regard to evidence. Numerous evidence-based therapy options are available for the treatment of impaired middle ear ventilation and otitis media, the main therapeutic approach being antibiotic treatment. Compromised ventilation results in inflammatory middle ear disorders. Its key function is to ensure middle ear ventilation. 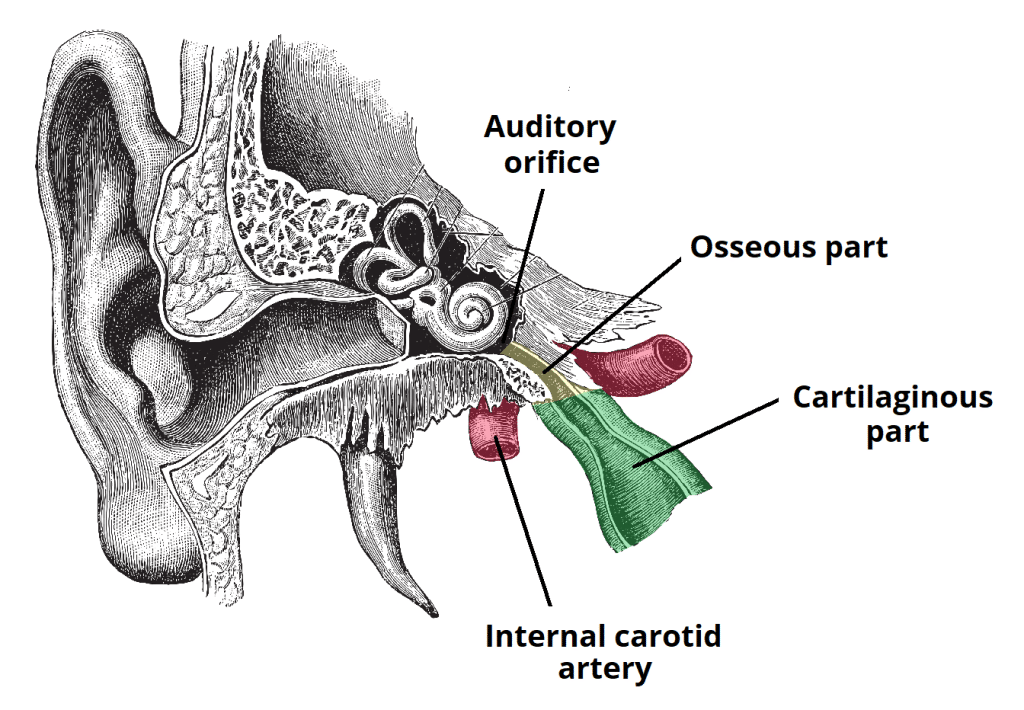
The Eustachian tube connects the nasopharynx with the middle ear cavity. For this purpose, a classification system has been established to categorize studies – and hence therapy options – in respect of associated evidence according to defined criteria. Evidence-based medicine is an approach to medical treatment intended to optimize patient-oriented decision-making on the basis of empirically proven effectiveness.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
